



Ireland’s Bovine TB Eradication Programme Advanced by Diagnostics
In the 1950s, Ireland set out to eradicate bovine tuberculosis (bTB). Today, they have a very successful bTB eradication programme in place that dramatically reduced production losses, maintained their export status and has helped their beef and dairy industry flourish.
“The foundation of the programme is surveillance underpinned by effective diagnostics, including annual testing of all live cattle in every herd in Ireland,” said Dr Margaret Good. “Thermo Fisher Scientific diagnostic tools, namely Tuberculin PPD and BOVIGAM, have been the diagnostic tools of choice for testing in live animals for many years, and thus these have helped Ireland to achieve its goals.”
Eradication Program Progress
In 1980, when Dr Good joined Ireland’s Department of Agriculture, Food and the Marine, the bTB eradication program had ceased to make any significant progress after the initial successful years. Countrywide, there were about 30,000 reactors (bTB-infected cattle) among a cattle population of 6.97 million. However, progress was at a standstill for a few reasons.
“Every cow was being tested then, just as they are today. The difference in 1980 would have been that we didn’t have BOVIGAM, and we were less strict in our diagnostic interpretation with the tuberculin skin test,” she said. “We also didn’t have the sophisticated systems that the department has now to analyze data, so we weren’t looking as critically at the risk factors or evaluating where the impediments to progress were impacting.”
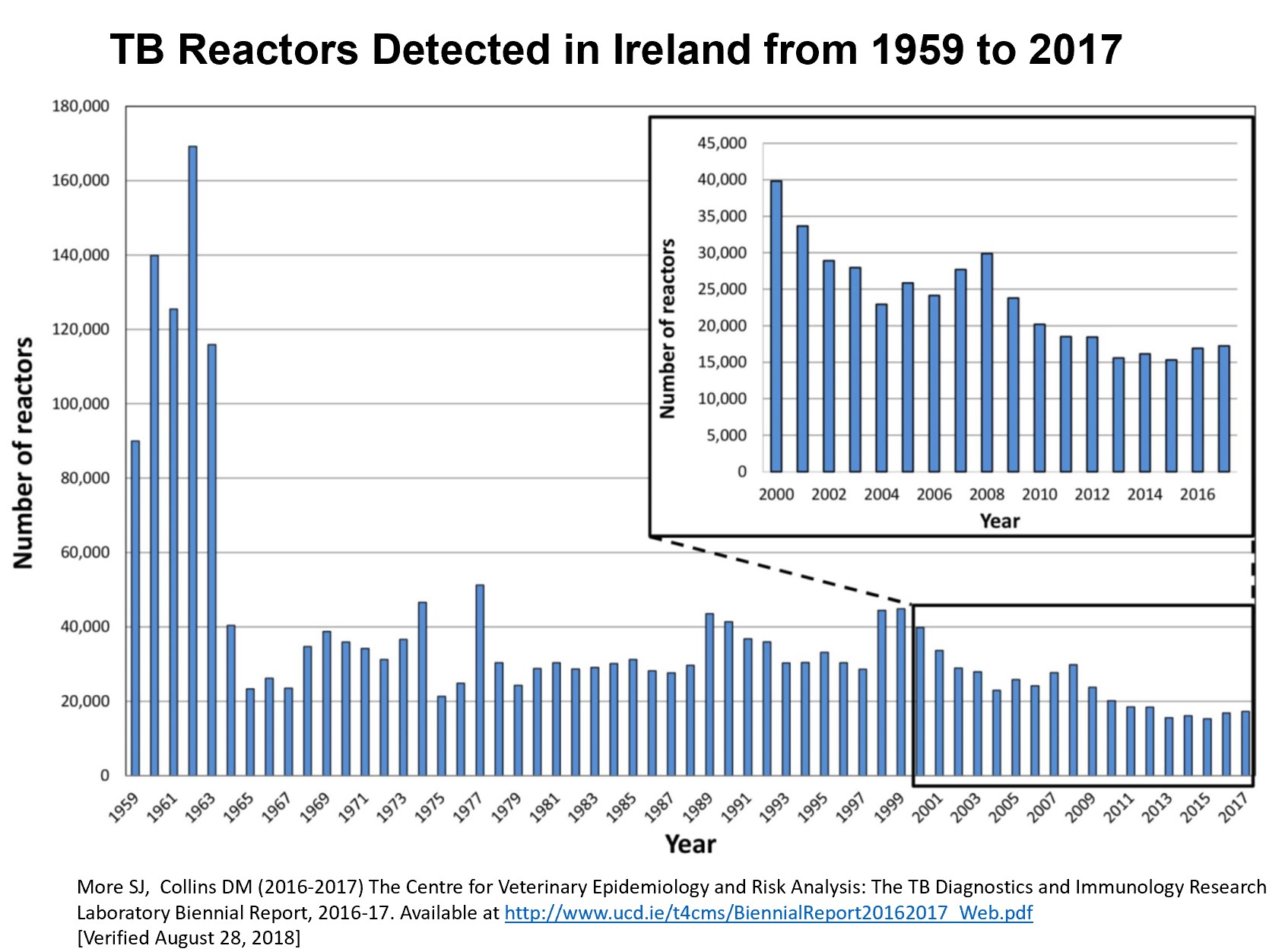
In the 1950s and 60s, the eradication program had made great strides. At the start of the program, well over 50% of bovine herds contained infected animals, and about 17% of the bovine population, including 22% of cows, were infected with bTB. Condemnation rates at slaughter were 2.3%, a rate considered very high.
“By 1965, the condemnation rate had fallen to 0.08%, and the animal bTB level had fallen from 17% to 0.44%, which involved culling 160,000 cattle in the peak year,” Dr Good noted. “The rapid progress led everyone to believe that eradication was possible in five to seven years—and then progress stalled.”
In 1975, the first TB-infected badger was identified. TB was later determined to be endemic in the badger population and caused by Mycobacterium bovis, which was also the dominant cause of bTB. Later still, it was found that both cattle and badgers shared the same strains of M. bovis. Since cattle and infected badgers share the pasture environment, TB-infected badgers and other wildlife were determined to be a significant constraint to TB eradication in cattle.
Boosting Progress Again
In 1987, Ireland was using two sets of bovine tuberculin purified protein derivative (PPD): 20,000 international units (IU) per ml with one mg of protein per ml, and 40,000 IU with two mg of protein per ml. The then-head of bTB research for the eradication program in the laboratory was reviewing the positive predictive value of the tests, including sensitivity and specificity.
“Intuitively, you would expect the higher-potency tuberculin to be more sensitive but less specific. However, he found that it was both more sensitive and more specific,” Dr Good says. “In the early 90s, we chose to use 30,000 IU bovine tuberculin and matched it with 25,000 IU avian tuberculin, so we could get consistently high sensitivity and specificity in the program. The product is very safe to use, and Ireland has tested many young calves on the day of birth if the herd was being tested that day. And Ireland is still using the product.”
When working with a TB-infected herd, Dr. Good said that to increase sensitivity, they routinely changed the interpretation level of the skin test, making it more severe, because the goal in Ireland is to eradicate bTB when it is found. To screen for bTB in a clean population, specificity is more important. They found that for specificity reasons, the comparative test was needed in Ireland for screening, but that it is still very sensitive in finding bTB-infected herds.
Progress took a step forward in 1999 when a computerized system, put in place in 1996, was fully operational under the European bovine identification legislation, whereby every animal is identified at birth and maintains that identification for life. Animal movements also then became recorded in the computer system, so there was full traceability linked to and integrated with the data for the bTB eradication program.
“This has helped make it much quicker to get back to the herd or herds through which an infected animal passed that might be the source of the infection,” Dr Good noted.
“In 2005, we officially recognized BOVIGAM as a test in the eradication program in Ireland and made it an integral part of the program for bTB-infected herds,” she said. “We also know from our data that cattle which tested negative to the skin test and positive to the BOVIGAM were 10 times more likely over the next 18 months to fail a skin test or confirm positive with bTB than their negative cohorts—and would continue to be so much longer than the 18 months. That’s why the test became legally compulsory when required for use in bTB-infected herds.”
If an animal does test positive in a herd, trade and cattle movement restrictions are immediately put on the farm. Dr Good says that if there’s an indication that an animal or group of animals is infected with bTB, it’s better to remove it earlier rather than leave it to result in further restrictions later. Every time a new positive animal is found, it results in new restrictions in the herd.
Current Tuberculosis Program
Because the ongoing bTB program has proven it still provides protection to the country’s cattle population, every herd and every bovine in Ireland is routinely tested for TB at least once a year. Infected herds are monitored and receive additional tests until they are clear.
.jpg) Tuberculin potency is hugely important, and for many years Ireland has confirmed the potency of the bovine tuberculin it uses through quality control checks at least two or three times a year in bTB infected cattle, to ensure it continues to perform properly.
Tuberculin potency is hugely important, and for many years Ireland has confirmed the potency of the bovine tuberculin it uses through quality control checks at least two or three times a year in bTB infected cattle, to ensure it continues to perform properly.
“In the 1970s, we got caught with some very low-potency tuberculin from suppliers we had at that time, so we learned the hard way,” said Dr Good. “Now, Ireland is probably the only country that routinely checks potency in naturally infected cattle. The Tuberculin PPD we use now is very specific; we get very few false positives in a herd, and we maintain a monitor of performance in specific ‘singleton herds’ to ensure specificity is maintained. We have run tenders every three to five years for supply, and the same company has been successful since we started, and we’re very satisfied that we use a good-quality tuberculin.”
Thermo Fisher Scientific diagnostic tools like Tuberculin PPD and BOVIGAM have been tested and have consistently met the program’s specifications.
“I interacted with the Thermo Fisher Scientific tuberculin production team for many years, and they are a very professional and dedicated to producing a quality product,” she said. “Every year, the Irish bTB eradication team has at least one site visit to the Thermo Fisher manufacturing facility, which always includes an open discussion.”
Beyond product quality, using BOVIGAM helps farmers reduce the duration of the restriction period and get cleared faster. Once positive animals are identified and the herd is recognized as bTB-infected, the target is that within 7 to 14 days, all cattle in the cohort will also be tested.
“The idea is that it maximizes the probability of all the infected animals being identified for removal in a short time frame, which can help reduce the duration of the restriction period that the farmer experiences. If we can reduce the restriction period by even two months, that’s significant for the farmer,” Dr Good explained.
As noted before, the data indicate that herds with animals who pass the skin test but fail the BOVIGAM test are 10 times more likely to diagnose positive for bTB. Taking this extra testing step should reduce the possibility of the herd having a repeated breakdown because one of these animals fails a subsequent test or is discovered at routine slaughter. Preventing another breakdown is perhaps even more significant for the farmer.
 “Getting to test quickly is very important, and a lot of farmers are now realizing that as well. They want the test done so they can be cleared as quickly as possible,” she said. “They want to be able to trade again. For them, it’s very important.”
“Getting to test quickly is very important, and a lot of farmers are now realizing that as well. They want the test done so they can be cleared as quickly as possible,” she said. “They want to be able to trade again. For them, it’s very important.”
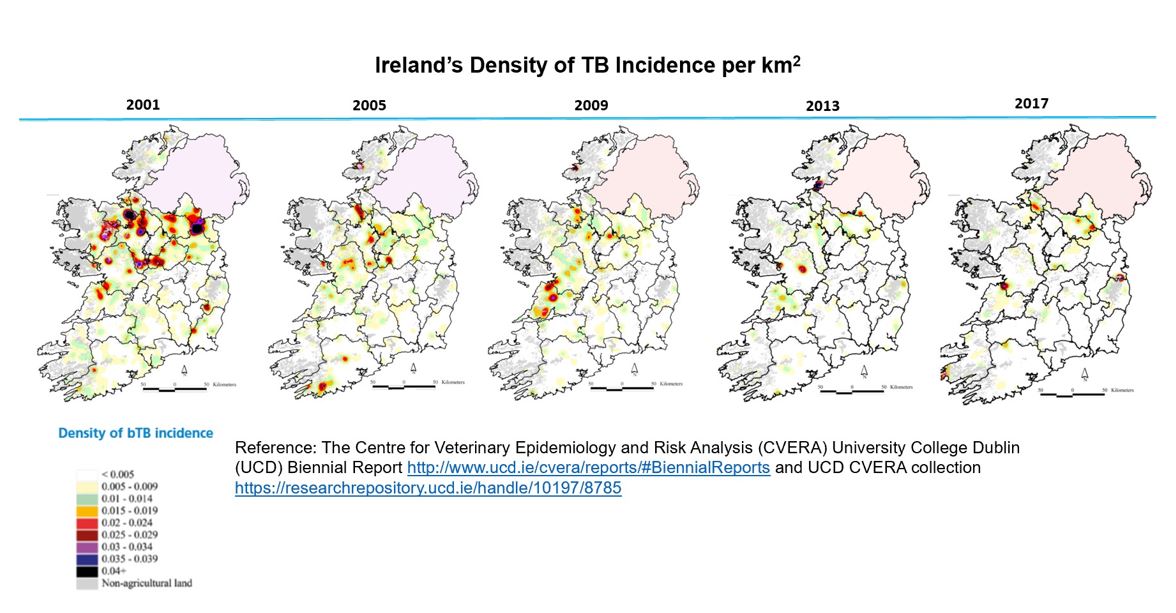
The bTB situation in Ireland has been making steady progress since the early 2000s, and the general disease trend is downward. At the end of 2017, there were 17,200 reactors for the year under the strict testing regime.
“We have done quite a lot of BOVIGAM testing, which has resulted in removing a lot of the positives in infected herds. That has put reactor numbers over and above what it would be if we were using just skin tests,” she explained. “But the expectation is that it will have benefits in succeeding years: the animals that are being removed will not turn up as infected in future years; this will reduce the number of herds restricted and it will reduce the spread of infection as well.”
Eradication, however, can’t be accomplished without addressing wildlife, according to Dr Good. As early as 1958, John Francis, a British veterinarian who later joined the staff at the University of Queensland where he continued his work on bTB, had recommended that to achieve complete eradication, TB had to be dealt with in all species where it occurred. Thus, Ireland needs to find a way to deal with TB in wildlife if the program is to achieve its ultimate goal of bTB eradication.
“Vaccination of wildlife should be a priority. We currently have an injectable vaccine, but it requires capture of badgers first and then injection. There is research ongoing into developing oral vaccination and delivery systems, which could be our most successful option to get vaccine to badger cubs as early as possible and protect them from becoming infected with M. bovis.”
Drivers for the Eradication Program
Several significant issues culminated in the 1950s to push the Irish government to start the eradication program:
- Economic losses: Farmers were suffering significant production losses to bTB. Previously, if you sent 100 animals to slaughter, at least two of them were going to be totally condemned, so they were a complete financial loss. Others would be partially condemned.
- Human health: Because pasteurization wasn’t generally initiated and regulated in Ireland until 1957, bTB-infected milk, especially in rural and farming communities, was moving into the consumer food supply and creating a human health risk.
- Stigma: In the late 19th century, TB had been the greatest health problem in young adults in Ireland, causing more than 11,500 deaths/year. Before the bTB eradication program commenced, many farmers’ children had TB, and some were unfortunate enough to have scrofula, a disease that can severely swell glands in the necks of humans who are infected. The infection was often caused on farms by drinking raw milk infected with Mycobacterium bovis. Since children generally drank more milk, they were the most likely to become infected. Many families with TB felt stigmatized in their locality.
- Export status: Ireland was an exporter of live cattle, and about 20% were going to England, where an eradication program had already been set up. There was a risk of losing export status if Irish store cattle couldn’t be of attested status (certified clear of the disease).
“A veterinarian who practiced in the early years of the bTB eradication program said he could look at the children, and if he saw scrofula, know before he ever tested the cattle that he was going to find a lot of reactors,” Dr Good noted. “He would also know, therefore, that every calf would have also been drinking bTB milk, and so most of the younger stock were going to be infected. So a lot of the herd was potentially infected, and that would be devastating for the farmer.”
Many organizations, like the Irish Red Cross, campaigned for a cattle eradication program because of the human health issues. A voluntary program was initiated in 1950, and many farmers were volunteering to test their cattle.
“It was clearly evident that during the voluntary phase, the industry was seeing improvements,” she said. “Then in September 1954, the program was made compulsory, although it took until 1962 to extend throughout the whole country. By 1965, it was already becoming quite rare to find cattle clinically affected by TB.”
Explore the Thermo Fisher Scientific Animal Health portfolio and our 50+ Years of Expertise. Applied.
Image sources:
Ireland’s density of TB Incidence per km2: The Centre for Veterinary Epidemiology and Risk Analysis (CVERA) University College Dublin (UCD) Biennial Report and the UCD CVERA collection.TB Reactors Detected in Ireland from 1959 to 2017: More S.J., and Collins, D.M. (2016-2017) The Centre for Veterinary Epidemiology and Risk Analysis: The TB Diagnostics and Immunology Research Laboratory Biennial Report, 2016–17. For Veterinary Use Only. For In Vitro use only. Regulatory requirements vary by country; products may not be available in your geographic area. In the US, these products are only available with a research and evaluation permit.



